
Logical Definition
If getting pregnant has been a challenge for you and your partner, you're not alone. Ten to 15 percent of couples in the United States are infertile. Infertility is defined as not being able to get pregnant despite having frequent, unprotected sex for at least a year for most people and six months in certain circumstances. Infertility may be due to a single cause in either you or your partner, or a combination of factors that may prevent a pregnancy from occurring or continuing. Fortunately, there are many safe and effective therapies for overcoming infertility. These treatments significantly improve the chances of becoming pregnant.
Infertility is a disease that results in the abnormal functioning of the male or female reproductive system. The American Society for Reproductive Medicine (ASRM) and the American College of Obstetricians and Gynecologists (ACOG) and the World Health Organization (WHO) recognize infertility as a disease.
The Top Ten Things I Learned About Infertility
After three years, I am stepping aside as the leader of the Chicago Northside Fertility Support Group—a group I deliberately called a Fertility Support Group (vs. Infertility) to focus on the positive side of this journey.
I looked into being a volunteer host after my son was born because I felt like a bit of a fraud when I hung out with other new moms. To them, I was just another lady with a baby. But, of course, there is so much more to our story than that. I see now that leading the group was a way for me to support other women struggling with infertility and also a way for me to find closure and move on to the next stage in my life. For me, after a five year struggle, nine months wasn't nearly long enough to move from infertility to motherhood. Having a child doesn't erase infertility; much as arriving at a destination doesn’t eliminate the journey.
In saying goodbye to the women in our group, I put together this Top Ten List, to share what we all know, but sometimes can’t find the words to say. Our group will continue; a new host will guide the group to keep listening, laughing, and traveling this road. Good luck, everyone. If you've had success and have your miracle child, or if you are still on your journey, think about volunteering as a RESOLVE leader. It may be just what you need to help others, and in the end, help yourself too.
Top Ten Things I Learned About Infertility (from a retiring volunteer support group leader)
Understand why it’s important to set realistic goals and develop an awareness of stressors and stress.
Coping Techniques
If getting pregnant has been a challenge for you and your partner, you're not alone. Ten to 15 percent of couples in the United States are infertile. Infertility is defined as not being able to get pregnant despite having frequent, unprotected sex for at least a year for most people and six months in certain circumstances. Infertility may be due to a single cause in either you or your partner, or a combination of factors that may prevent a pregnancy from occurring or continuing. Fortunately, there are many safe and effective therapies for overcoming infertility. These treatments significantly improve the chances of becoming pregnant.
Infertility is a disease that results in the abnormal functioning of the male or female reproductive system. The American Society for Reproductive Medicine (ASRM) and the American College of Obstetricians and Gynecologists (ACOG) and the World Health Organization (WHO) recognize infertility as a disease.
The Top Ten Things I Learned About Infertility
After three years, I am stepping aside as the leader of the Chicago Northside Fertility Support Group—a group I deliberately called a Fertility Support Group (vs. Infertility) to focus on the positive side of this journey.
I looked into being a volunteer host after my son was born because I felt like a bit of a fraud when I hung out with other new moms. To them, I was just another lady with a baby. But, of course, there is so much more to our story than that. I see now that leading the group was a way for me to support other women struggling with infertility and also a way for me to find closure and move on to the next stage in my life. For me, after a five year struggle, nine months wasn't nearly long enough to move from infertility to motherhood. Having a child doesn't erase infertility; much as arriving at a destination doesn’t eliminate the journey.
In saying goodbye to the women in our group, I put together this Top Ten List, to share what we all know, but sometimes can’t find the words to say. Our group will continue; a new host will guide the group to keep listening, laughing, and traveling this road. Good luck, everyone. If you've had success and have your miracle child, or if you are still on your journey, think about volunteering as a RESOLVE leader. It may be just what you need to help others, and in the end, help yourself too.
Top Ten Things I Learned About Infertility (from a retiring volunteer support group leader)
- Infertility is linear...you don’t know how you’re going feel about any treatment or any part of it until you get there. One minute you may say “no way” to IVF, and then you find yourself giving yourself shots and counting follicles!
- Men (husbands/partners) do care, and they will be great fathers. But, in my experience, I've noticed that their highs are not as high nor are their lows as low on the path to parenthood. Most of them are able to picture life without children without tears coming to their eyes and can easily see how life with more money and no children can be a viable version of a happy ending. I don’t completely buy the conventional explanation of “it’s not happening to their body.” I think it’s more that many of them are Cubs fans and are used to painful disappointment for the team they love.
- There’s no dipping your toe into the infertility world. You’re either underwater or by the side of the pool.
- You cannot understand this until you go through it. Period.
- Pick a few people to talk to this about, and then forgive them if they ask you how it’s going when you don’t want to talk about it. Letting people in and talking about this pain can really ease the burden, but once they’re in, they’re in -- no two ways about it.
- Baby showers, baby pictures, hearing moms complain about their kids -- these are all things that can, and probably should, be removed from your life for the time being.
- Jealousy and intense dislike (I intensely dislike the word hate) are a natural part of the human rainbow of emotions. Feel them, forgive yourself, and move on.
- It’s likely that not all relationships in your life will survive infertility. Friends who get pregnant while you can’t may be casualties. It happens.
- Have talking points when you go to Christmas dinner....or just out for coffee. When people ask if you have kids or if you plan to, have something ready to say, so you don’t have to think on your feet. Mine were: “It doesn't look like it’s in the cards for us.” That seemed to make people feel a little bad for asking (which I have to admit I wanted) and let folks know we’d tried, which, for some reason, I also wanted.
- Nothing stresses a woman out more than being told to relax. This is not your fault.
Understand why it’s important to set realistic goals and develop an awareness of stressors and stress.
Coping Techniques
The Body
Why it is importantOur bodies are incredible machines that have the ability to tell us when something is wrong. But in order to recognize the warnings signs we must understand how our bodies feel when everything is functioning normally. When you get a headache your body is sending you a signal that it is off kilter. In order to treat this headache you can take various forms of over the counter pain relievers, try alternative medicinal efforts such as meditation/relaxation or simply ignore it. If you pay attention to the headache and notice a pattern, it may help you prevent something more serious. It may even help you recognize when you are under stress, and how that stress is adversely affecting your health.
Your fertility is a key function of this machine. It is critical to understand your fertility to help preserve it and to help ensure your good health. Understanding your fertility may help to prevent infertility. It will also help you understand what is happening as you are trying to conceive naturally, by helping you optimize your fertile periods. Most importantly, understanding fertility for both men and women will help them feel in control when they are faced with infertility.
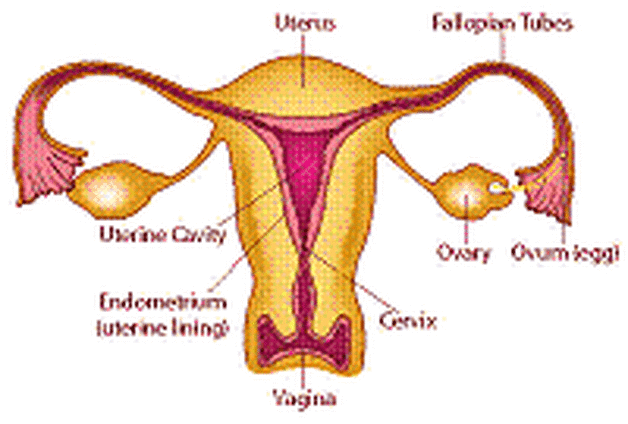
The Female Reproductive System
The female reproductive system includes the following organs and glands:
Ovaries
Thick, muscular organ that is designed to support a growing fetus
Endometrium
A ring of tissue at the top of the vagina designed to collect sperm (with a cervical mucus), which are later released into the uterus.
Observing changes in your cervical mucus will help you determine signs of fertility
Vagina
Sperm enter the woman's body through the vagina which then leads to the cervix.
The Menstrual Cycle
Understanding What Happens Not every woman experiences a standard 28-day cycle. Some women may have longer or shorter cycles and still be fertile.
Day 1
The first day of your cycle is the first day of blood flow. Some women bleed for 3-6 days, others 2-3 days. It is not unusual to have some light spotting before the menstrual period.
Days 2-14
This is called the follicular phase. During this time, the endometrium starts to grow, the follicles on the ovary become active, and the cervical mucous begins to thin.
Day 14
Ovulation takes mid cycle. Rising estrogen levels trigger the release of LH (the “LH” surge). The climbing level of LH causes the follicle to ovulate, releasing an egg. The timing of ovulation is not precise; it may occur between days 12 and 14, depending on the individual woman. That is why it is important to understand and chart your cycle (record your basal body temperature and your LH surge on an ovulation test kit).
Days 15-22
After releasing the egg, the follicle transforms into the corpus luteum, and progesterone is released, creating a lush uterine lining for implantation. This stage of the cycle is called the luteal phase.
Days 23 to 24
If there is no implantation, estrogen and progesterone levels fall.
Days 25 to 28
The falling progesterone levels trigger the shedding of the endometrium.
Tracking Most Fertile Time
Basal Body Temperature (BBT)
Keeping track of your BBT is a way to document whether you have ovulated. A specific hormonal change during your cycle triggers a rise in basal body temperature. By taking your temperature every day you can chart the rise of your temperature and the day you ovulate. The BBT chart will not predict when you are going to ovulate, but can serve as a record of your patterns. This will be helpful information for your physician. Ovulation predictor kits are designed to help you predict the time you will ovulate.
Ovulation Predictor Kits
Urine test kits to monitor luteinizing hormone (LH) are called ovulation predictor kits. They are designed to help you predict the time you will ovulate so that you can maximize your chances of getting pregnant. Most kits typically require you to perform a simple urine test. When you urinate on a special stick from this kit, it will document the surge of LH released by the pituitary just before ovulation, usually 24-38 hours before the egg is released. Most kits offer clear instructions for use and a toll-free number to call if you have questions.
Understanding Ovulation
The Egg When a girl is born, she typically has between 1 and 2 million eggs in her ovaries (primary oocytes.) She will begin to lose these eggs early in life leaving her only 300,000 to 500,000 by the age of puberty.
As the eggs are formed, thin layers of cells (granulosa cells) grow around them. The granulosa cells and the oocyte are contained within a follicle. The follicle supports the egg it encloses for 50 years or more, providing it with nourishment but preventing it from maturing. The great majority of follicles and eggs never grow to maturity and ovulation. Follicles begin to develop, but if conditions for continued growth are not optimal, the eggs lose nourishment and die. The follicle cells then are absorbed back into the ovary (atresia.) Atresia continues throughout a woman's life until all of the follicles are gone and she enters menopause.
During the hours leading up to ovulation when the mature egg is released from the dominant follicle, some important processes begin:
The Male Reproductive System
The male reproductive system includes the following organs and glands:
Scrotum
Conception
An Incredible Confluence of Events The Woman
Must release a healthy, mature ovum, which must be picked up by a healthy, functional fallopian tube
The Man
Must produce healthy sperm and deposit it in the vagina, near the cervical opening. (once deposited, only about 10% of the sperm survive to penetrate the cervical mucous)
The Couple
Must have intercourse every other day around the time of ovulation, because sperm live for only about 48 hours.
Fertilization
Sperm must make it through the cervix and through the uterus into the fallopian tube. One healthy sperm must breach the egg's protective layers, including the cumulus layer and the zona pellucida.
Progesterone and pregnancy: a vital connection
Progesterone is a natural female hormone. Called “the pregnancy hormone,” it is essential before and during pregnancy.
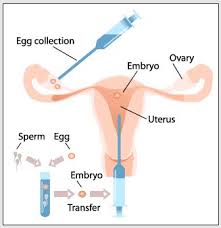
Progesterone supplementation is often necessary during Assisted Reproductive Technology (ART) procedures, such as in-vitro fertilization (IVF) because the medications you may use during these procedures can suppress your body’s ability to produce progesterone. Certain procedures can even, inadvertently, remove progesterone-producing cells from your ovaries.
Sometimes, there are other reasons to use progesterone supplementation, such as little or no progesterone production from the ovaries or poorly developed follicles that do not secrete enough progesterone to develop the uterine lining.
The bottom line is this — all women who wish to become pregnant need progesterone to help the uterus prepare for and maintain a fertilized egg. Follow the links below to learn more about the connection between progesterone and pregnancy.
After ovulation occurs, the ovaries start to produce progesterone needed by the uterus. Progesterone causes the uterine lining or endometrium to thicken. This helps prepare a supportive environment in your uterus for a fertilized egg.
Why it is importantOur bodies are incredible machines that have the ability to tell us when something is wrong. But in order to recognize the warnings signs we must understand how our bodies feel when everything is functioning normally. When you get a headache your body is sending you a signal that it is off kilter. In order to treat this headache you can take various forms of over the counter pain relievers, try alternative medicinal efforts such as meditation/relaxation or simply ignore it. If you pay attention to the headache and notice a pattern, it may help you prevent something more serious. It may even help you recognize when you are under stress, and how that stress is adversely affecting your health.
Your fertility is a key function of this machine. It is critical to understand your fertility to help preserve it and to help ensure your good health. Understanding your fertility may help to prevent infertility. It will also help you understand what is happening as you are trying to conceive naturally, by helping you optimize your fertile periods. Most importantly, understanding fertility for both men and women will help them feel in control when they are faced with infertility.
The Female Reproductive System
The female reproductive system includes the following organs and glands:
Ovaries
- Produce female hormones: estrogen and progesterone
- Produce one ripened egg (called ovum) each menstrual cycle
- Each month one of the ovaries produces an egg, which develops in a small fluid-filled sac called the follicle. When the egg is mature it is released from the ovary and passes through one of the fallopian tubes.
- Two trumpet shaped, flexible tubes connected to the uterus, they are designed with flared projections (fimbriae) to catch the egg and move it into the tube.
- Egg and sperm meet in the fallopian tubes and it is here that the egg becomes fertilized and the resulting embryo is transferred to the uterus by cilia (small hairlike structures)
Thick, muscular organ that is designed to support a growing fetus
Endometrium
- Mucous membrane that lines the uterus and plays a key role in implantation of the embryo.
- The endometrium responds to the hormone progesterone, produced by the body and must be thick and spongy to receive the embryo. If there is not implantation the lining is shed with a menstrual period.
A ring of tissue at the top of the vagina designed to collect sperm (with a cervical mucus), which are later released into the uterus.
Observing changes in your cervical mucus will help you determine signs of fertility
Vagina
Sperm enter the woman's body through the vagina which then leads to the cervix.
The Menstrual Cycle
Understanding What Happens Not every woman experiences a standard 28-day cycle. Some women may have longer or shorter cycles and still be fertile.
Day 1
The first day of your cycle is the first day of blood flow. Some women bleed for 3-6 days, others 2-3 days. It is not unusual to have some light spotting before the menstrual period.
Days 2-14
This is called the follicular phase. During this time, the endometrium starts to grow, the follicles on the ovary become active, and the cervical mucous begins to thin.
Day 14
Ovulation takes mid cycle. Rising estrogen levels trigger the release of LH (the “LH” surge). The climbing level of LH causes the follicle to ovulate, releasing an egg. The timing of ovulation is not precise; it may occur between days 12 and 14, depending on the individual woman. That is why it is important to understand and chart your cycle (record your basal body temperature and your LH surge on an ovulation test kit).
Days 15-22
After releasing the egg, the follicle transforms into the corpus luteum, and progesterone is released, creating a lush uterine lining for implantation. This stage of the cycle is called the luteal phase.
Days 23 to 24
If there is no implantation, estrogen and progesterone levels fall.
Days 25 to 28
The falling progesterone levels trigger the shedding of the endometrium.
Tracking Most Fertile Time
Basal Body Temperature (BBT)
Keeping track of your BBT is a way to document whether you have ovulated. A specific hormonal change during your cycle triggers a rise in basal body temperature. By taking your temperature every day you can chart the rise of your temperature and the day you ovulate. The BBT chart will not predict when you are going to ovulate, but can serve as a record of your patterns. This will be helpful information for your physician. Ovulation predictor kits are designed to help you predict the time you will ovulate.
Ovulation Predictor Kits
Urine test kits to monitor luteinizing hormone (LH) are called ovulation predictor kits. They are designed to help you predict the time you will ovulate so that you can maximize your chances of getting pregnant. Most kits typically require you to perform a simple urine test. When you urinate on a special stick from this kit, it will document the surge of LH released by the pituitary just before ovulation, usually 24-38 hours before the egg is released. Most kits offer clear instructions for use and a toll-free number to call if you have questions.
Understanding Ovulation
The Egg When a girl is born, she typically has between 1 and 2 million eggs in her ovaries (primary oocytes.) She will begin to lose these eggs early in life leaving her only 300,000 to 500,000 by the age of puberty.
As the eggs are formed, thin layers of cells (granulosa cells) grow around them. The granulosa cells and the oocyte are contained within a follicle. The follicle supports the egg it encloses for 50 years or more, providing it with nourishment but preventing it from maturing. The great majority of follicles and eggs never grow to maturity and ovulation. Follicles begin to develop, but if conditions for continued growth are not optimal, the eggs lose nourishment and die. The follicle cells then are absorbed back into the ovary (atresia.) Atresia continues throughout a woman's life until all of the follicles are gone and she enters menopause.
During the hours leading up to ovulation when the mature egg is released from the dominant follicle, some important processes begin:
- The production of the LH hormone (lutenizing hormone rises in the blood).
- A few hours before ovulation, the primary oocyte undergoes a cell division process (meiosis) which results in an egg that contains 23 chromosomes
- The follicle cells surrounding the oocyte secrete mucous, forming a circular barrier (the cumulus) around the oocyte. Beneath the cumulus is a glassy looking membrane the zona pellucida. Sperm must be able to go through the cumulus and the zona pellucida of the egg in order to fertilize it.
- The egg is released and is picked up by the fimbriated ends of the fallopian tube.
- Fertilization usually occurs in the fallopian tube 12-24 hours after ovulation.
The Male Reproductive System
The male reproductive system includes the following organs and glands:
Scrotum
- Contains the testes, the sperm producing organs
- The location of the scrotum, outside the body, behind the penis, help to maintain the temperature, ensuring normal sperm production.
- Oval glands located within the scrotum
- Produce testosterone
- Produce sperm cells
- Produce testosterone
- Produce growth factors that nourish sperm.
- Store sperm for about 3 months
- This is where sperm begin to mature
- Long coiled tube that lies beside and behind the testes
- Helps sperm mature fully (after the seminiferous tubules) and transports them to the vas deferens
- Sperm remain here for 2-12 days
- Long tube with thick walls, it runs from the end of the epididymis upward into the pelvis behind the bladder.
- Contribute the seminal fluid and produce the sugar fructose, which the sperm use to fuel their long journey
- Contribute additional fluid and important enzymes that cause semen to liquefy after ejaculation
- Located beyond the prostate at the base of the penile shaft in the urethra
- Adds a small amount of lubricant to the seminal fluid before ejaculation takes place
- The penis allows the man to deposit the seminal fluid into the vagina.
Conception
An Incredible Confluence of Events The Woman
Must release a healthy, mature ovum, which must be picked up by a healthy, functional fallopian tube
The Man
Must produce healthy sperm and deposit it in the vagina, near the cervical opening. (once deposited, only about 10% of the sperm survive to penetrate the cervical mucous)
The Couple
Must have intercourse every other day around the time of ovulation, because sperm live for only about 48 hours.
Fertilization
Sperm must make it through the cervix and through the uterus into the fallopian tube. One healthy sperm must breach the egg's protective layers, including the cumulus layer and the zona pellucida.
Progesterone and pregnancy: a vital connection
Progesterone is a natural female hormone. Called “the pregnancy hormone,” it is essential before and during pregnancy.
Progesterone supplementation is often necessary during Assisted Reproductive Technology (ART) procedures, such as in-vitro fertilization (IVF) because the medications you may use during these procedures can suppress your body’s ability to produce progesterone. Certain procedures can even, inadvertently, remove progesterone-producing cells from your ovaries.
Sometimes, there are other reasons to use progesterone supplementation, such as little or no progesterone production from the ovaries or poorly developed follicles that do not secrete enough progesterone to develop the uterine lining.
The bottom line is this — all women who wish to become pregnant need progesterone to help the uterus prepare for and maintain a fertilized egg. Follow the links below to learn more about the connection between progesterone and pregnancy.
- Before pregnancy
- During pregnancy
- Forms of progesterone
- Choosing the progesterone supplementation for you
After ovulation occurs, the ovaries start to produce progesterone needed by the uterus. Progesterone causes the uterine lining or endometrium to thicken. This helps prepare a supportive environment in your uterus for a fertilized egg.
Am I Fertile? Am I Ovulating? Am I Pregnant?
Content originally provided by Church & Dwight, makers of First Response.
While many women think that getting pregnant will be no trouble, millions of women in America struggle with infertility. According to a new survey conducted by RESOLVE, 70 percent of women who may want to have children think they can get pregnant whenever they want. But according to the Center of Disease Control and Prevention, infertility affects 7.3 million Americans.
“My patients frequently ask me about those life-changing questions in a woman’s reproductive cycle: Am I fertile? Am I ovulating? Am I pregnant?” said Dr. Peter Ahlering, M.D., a St. Louis based OB/GYN and Medical Director at SIRM-St. Louis.
Am I fertile?
Every woman is born with all of the eggs that she will ever have. Each month one or more eggs will mature in the ovaries in preparation for ovulation. As the eggs mature and are released over time, the number of eggs, which is a measure of your fertility potential, decreases.
Follicle Stimulating Hormone, (FSH), is one of many hormones that your body uses to regulate your menstrual cycle and to control the maturation of your eggs. FSH signals the ovaries to mature one or more eggs for ovulation each month/cycle.
If your ovarian reserve (eggs) is low in quantity or quality, your pituitary will produce higher than normal FSH levels early in the cycle trying to stimulate your ovaries to produce a mature egg. In other words, when your quantity or quality of eggs (your fertility potential) is low, your FSH level may be high.
Therefore, knowing your FSH level on Day 3 of the menstrual cycle can be helpful in finding out your fertility potential.
FSH is one of the leading single indicators of a woman’s fertility potential and now it is possible to gauge your fertility potential through a simple at-home test.
Am I Ovulating?
There are only about 2 days a month when are you most likely to get pregnant. Identify the most fertile days within your cycle and then plan intercourse to correspond with these times of peak fertility.
Am I pregnant?
At-Home Pregnancy Tests detect the pregnancy hormone hCG (Human Chorionic Gonadotropin) in urine as early as 5 days before missed period. Knowing sooner is important! The sooner you know you’re pregnant, the sooner you can take better care of yourself and your developing baby.
This section of the RESOLVE website is made possible in part by support from Church & Dwight Co., Inc., makers
Content originally provided by Church & Dwight, makers of First Response.
While many women think that getting pregnant will be no trouble, millions of women in America struggle with infertility. According to a new survey conducted by RESOLVE, 70 percent of women who may want to have children think they can get pregnant whenever they want. But according to the Center of Disease Control and Prevention, infertility affects 7.3 million Americans.
“My patients frequently ask me about those life-changing questions in a woman’s reproductive cycle: Am I fertile? Am I ovulating? Am I pregnant?” said Dr. Peter Ahlering, M.D., a St. Louis based OB/GYN and Medical Director at SIRM-St. Louis.
Am I fertile?
Every woman is born with all of the eggs that she will ever have. Each month one or more eggs will mature in the ovaries in preparation for ovulation. As the eggs mature and are released over time, the number of eggs, which is a measure of your fertility potential, decreases.
Follicle Stimulating Hormone, (FSH), is one of many hormones that your body uses to regulate your menstrual cycle and to control the maturation of your eggs. FSH signals the ovaries to mature one or more eggs for ovulation each month/cycle.
If your ovarian reserve (eggs) is low in quantity or quality, your pituitary will produce higher than normal FSH levels early in the cycle trying to stimulate your ovaries to produce a mature egg. In other words, when your quantity or quality of eggs (your fertility potential) is low, your FSH level may be high.
Therefore, knowing your FSH level on Day 3 of the menstrual cycle can be helpful in finding out your fertility potential.
FSH is one of the leading single indicators of a woman’s fertility potential and now it is possible to gauge your fertility potential through a simple at-home test.
Am I Ovulating?
There are only about 2 days a month when are you most likely to get pregnant. Identify the most fertile days within your cycle and then plan intercourse to correspond with these times of peak fertility.
- Every month an egg matures, leaves the ovary and travels down one of your fallopian tubes. This is called “ovulation”.
- Ovulation is primarily triggered by a monthly surge in a hormone referred to as “LH” (Luteinizing Hormone). The level of LH rises during the 24-36 hours before ovulation this is the “LH Surge”.
- Your best chance to become pregnant occurs when you have intercourse within 24-36 hours after the LH surge.
- Women’s menstrual cycles can vary from 20-44 days. This means the day of the month you ovulate can vary significantly. Most women do not ovulate mid-cycle. With so much variability, it may be difficult for a woman to find her peak fertility.
- Become familiar with your cycle by using ovulation tests before you’re actually ready to get pregnant. Ovulation Tests help you to identify the timing of your “LH Surge”: †
Am I pregnant?
At-Home Pregnancy Tests detect the pregnancy hormone hCG (Human Chorionic Gonadotropin) in urine as early as 5 days before missed period. Knowing sooner is important! The sooner you know you’re pregnant, the sooner you can take better care of yourself and your developing baby.
This section of the RESOLVE website is made possible in part by support from Church & Dwight Co., Inc., makers

How Do I Know if I Have an Infertility Problem?
If you are trying to have a baby and it is not happening as quickly as you expected, you may wonder if you have an infertility issue. This section is designed to determine if you should see an infertility specialist.
Is infertility a "woman's" problem?
Infertility is a medical problem. Approximately 30% of infertility is due to female factor and 30% is due to male factor. In the balance of the cases, infertility results from problems in both partners or the cause of the infertility is "unexplained".
At what time of the month is a woman most fertile?
The day you start your menstrual period is "Day 1." Around "Day 14" you may ovulate and release an egg. The egg is viable for 24 hours; this is your most fertile time. However, not all women ovulate on "Day 14." Some ovulate earlier and some later. Some women do not ovulate at all. Your ovulation pattern can vary month to month. Even if you are getting your period, that does not mean you are ovulating. Read more about Ovulation here.
How can a woman tell when she ovulates?
One way of determining when you ovulate is to take your basal body temperature every morning and record it on a chart. Three or four months should be adequate to share with your doctor. You can also buy an ovulation predictor kit.
How often should we have intercourse?
Sperm can live for approximately 48 hours in the woman's reproductive tract. It is important to have sexual intercourse at this time. It is a good idea to have intercourse every other day around the time you ovulate. (Day 10, 12, 14, and 16.) Remember that every woman ovulates at a different time. To increase your chances of becoming pregnant, do not douche or use lubricants immediately before or after intercourse.
How long should we try before we see a doctor?
Most physicians advise you not to be concerned unless you have been trying to conceive for at least one year and are under 35. If you are over 35 and have been trying for 6 months, you should consult a physician. If you are over 30 and have a history of pelvic inflammatory disease, painful periods, miscarriage, irregular cycles, or if you know that your partner has a low sperm count, do not wait one year. Consult your ob/gyn.
Many couples have a difficult time admitting there may be a problem. After each menstrual cycle there is hope that "it will work this time." When these hopes are dashed month after month, you should consult your OB/GYN or contact with others through RESOLVE.
How do we find a good infertility specialist?
Many Ob/Gyns and Urologists are specially trained to treat the patient having difficulty conceiving. Doctors who specialize in infertility are board certified in reproductive endocrinology.
Related Articles:
If you are trying to have a baby and it is not happening as quickly as you expected, you may wonder if you have an infertility issue. This section is designed to determine if you should see an infertility specialist.
Is infertility a "woman's" problem?
Infertility is a medical problem. Approximately 30% of infertility is due to female factor and 30% is due to male factor. In the balance of the cases, infertility results from problems in both partners or the cause of the infertility is "unexplained".
At what time of the month is a woman most fertile?
The day you start your menstrual period is "Day 1." Around "Day 14" you may ovulate and release an egg. The egg is viable for 24 hours; this is your most fertile time. However, not all women ovulate on "Day 14." Some ovulate earlier and some later. Some women do not ovulate at all. Your ovulation pattern can vary month to month. Even if you are getting your period, that does not mean you are ovulating. Read more about Ovulation here.
How can a woman tell when she ovulates?
One way of determining when you ovulate is to take your basal body temperature every morning and record it on a chart. Three or four months should be adequate to share with your doctor. You can also buy an ovulation predictor kit.
How often should we have intercourse?
Sperm can live for approximately 48 hours in the woman's reproductive tract. It is important to have sexual intercourse at this time. It is a good idea to have intercourse every other day around the time you ovulate. (Day 10, 12, 14, and 16.) Remember that every woman ovulates at a different time. To increase your chances of becoming pregnant, do not douche or use lubricants immediately before or after intercourse.
How long should we try before we see a doctor?
Most physicians advise you not to be concerned unless you have been trying to conceive for at least one year and are under 35. If you are over 35 and have been trying for 6 months, you should consult a physician. If you are over 30 and have a history of pelvic inflammatory disease, painful periods, miscarriage, irregular cycles, or if you know that your partner has a low sperm count, do not wait one year. Consult your ob/gyn.
Many couples have a difficult time admitting there may be a problem. After each menstrual cycle there is hope that "it will work this time." When these hopes are dashed month after month, you should consult your OB/GYN or contact with others through RESOLVE.
How do we find a good infertility specialist?
Many Ob/Gyns and Urologists are specially trained to treat the patient having difficulty conceiving. Doctors who specialize in infertility are board certified in reproductive endocrinology.
Related Articles:

Healthy Living
It is not something you should worry about only when you are ready to have children, it is critical to think about lifestyle factors well before that. Infertility affects 7.3 million people. 30% of infertility is attributed to the male, while 30% is attributed to the female. 30% of infertility cases are due to weighing too much or too little. It is critical to understand your fertility and explore healthy lifestyle options in order to preserve and enhance your fertility.
Lifestyle factors that can have a negative long-term influence on your health and your fertility are as follows:
For example: Caffeine, a stimulant found in coffee, tea, soda and chocolate, has negative effects on health and fertility. Caffeine can increase stress and is known to have addictive qualities. Caffeine may cause damage to sperm and increases the risk in females of developing endometriosis. So, instead of reaching for that cup of coffee in the morning, try a cup of herbal tea and a glass of calcium fortified orange juice to reduce stress, reduce caffeine intake and optimize your health.
Related links:
Healthy Eating
One Woman's Personal Story
Relaxation and Stress Management for Infertile Women
It is not something you should worry about only when you are ready to have children, it is critical to think about lifestyle factors well before that. Infertility affects 7.3 million people. 30% of infertility is attributed to the male, while 30% is attributed to the female. 30% of infertility cases are due to weighing too much or too little. It is critical to understand your fertility and explore healthy lifestyle options in order to preserve and enhance your fertility.
Lifestyle factors that can have a negative long-term influence on your health and your fertility are as follows:
- Caffeine consumption
- Smoking
- Unprotected sex
- Overuse of alcohol
- Body weight
- Poor nutrition
For example: Caffeine, a stimulant found in coffee, tea, soda and chocolate, has negative effects on health and fertility. Caffeine can increase stress and is known to have addictive qualities. Caffeine may cause damage to sperm and increases the risk in females of developing endometriosis. So, instead of reaching for that cup of coffee in the morning, try a cup of herbal tea and a glass of calcium fortified orange juice to reduce stress, reduce caffeine intake and optimize your health.
Related links:
Healthy Eating
One Woman's Personal Story
Relaxation and Stress Management for Infertile Women
- What is infertility?
- Is infertility a common problem?
- Is infertility just a woman's problem?
- What causes infertility in men?
- What increases a man's risk of infertility?
- What causes infertility in women?
- What things increase a woman's risk of infertility?
- How does age affect a woman's ability to have children?
- How long should women try to get pregnant before calling their doctors?
- How will doctors find out if a woman and her partner have fertility problems?
- How do doctors treat infertility?
- What medicines are used to treat infertility in women?
- What is intrauterine insemination (IUI)?
- What is assisted reproductive technology (ART)?
- How often is assisted reproductive technology (ART) successful?
- What are the different types of assisted reproductive technology (ART)?
- Surrogacy
- Gestational carrier
GET PREGNANT WITHIN DAYS
Infertility facts
*Infertility facts medically edited by: Charles Patrick Davis, MD, PhD
What is infertility?
Comment on this Read 2 CommentsShare Your Story
Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to stay pregnant may also be infertile.
Pregnancy is the result of a process that has many steps. To get pregnant:
*Infertility facts medically edited by: Charles Patrick Davis, MD, PhD
- Infertility means not being able to become pregnant, within certain parameters.
- Infertility is a common problem of about 10% of women aged 15 to 44.
- Infertility can be due to the woman (33%), the man (33%) and by both sexes or due to unknown problems (33%), approximately.
- Infertility in men can be due to varicocele, low or absent sperm count, sperm damage or certain diseases.
- Risk factors for men's infertility include alcohol and drug use, toxins, smoking, age, health problems, medicines, radiation, and chemotherapy.
- Risk factors for women's infertility include ovulation problems, blocked Fallopian tubes, uterine problems, uterine fibroids, age, stress, poor diet, athletic training, and those risk factors listed for men.
- Aging decreases a woman's fertility; after age 35 about 33% of couples have fertility problems; older women's eggs are reduced in number, not as healthy and less likely to be released by the ovary – the woman is also more likely to have a miscarriage and other health problems.
- Women under 35 should try for a year or 6 months if 35 or older tobecome pregnant before contacting their doctor if they have no health problems.
- Doctors use the histories of both partners and may run tests such as sperm studies, ovulation tests, ultrasound, hysterosalpingography, orlaparoscopy.
- Infertility may be treated with medicine, surgery, artificial insemination, or assisted reproductive technology, based on the couples test results and other factors.
- There are multiple medicines that may be used to treat infertility in women.
- Intrauterine insemination is artificial insemination where a woman is injected with sperm into the uterus.
- ART (assisted reproductive technology) is when a woman's eggs are removed, mixed with sperm to make embryos that are placed back in the woman's body; it's successful about 11% to 39%, depending on the woman's age.
- There are several types of ART; in vitro fertilization, Zygote transfer, Gamete transfer and intracytoplasmic sperm injection.
- Surrogacy (the woman's male partner sperm is used to fertilize another woman egg and that other woman carries the fetus to term and the infant is then adopted ) is a way for some couples to obtain a baby.
- A gestational carrier is a woman who has an embryo placed in her uterus, carries the fetus to term and gives the baby to the couple (or responsible persons) that produced the embryo.
What is infertility?
Comment on this Read 2 CommentsShare Your Story
Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to stay pregnant may also be infertile.
Pregnancy is the result of a process that has many steps. To get pregnant:
- A woman must release an egg from one of her ovaries (ovulation).
- The egg must go through a Fallopian tube toward the uterus (womb).
- A man's sperm must join with (fertilize) the egg along the way.
- The fertilized egg must attach to the inside of the uterus (implantation).
This Sunday, fathers across the country will be pampered by their sons and daughters – they'll be encouraged to put their feet up and watch the World Cup on the television. Surrounded by their children, they'll be showered with gifts and love.
But for Irish men everywhere, the day will serve as a reminder of their difficulties in becoming fathers themselves.
"For many men, not being able to father a child is one of the biggest struggles they will face in their lifetime," says Helen Browne of the National Infertility Support and Information Group (NISIG). "Male infertility is often overlooked in favour of the emotional and physical toll fertility treatment takes on women. Often the men suffer in silence."
When Louis and his wife, who live in the midlands, married seven years ago, they planned to have a family. But, after two years of trying unsuccessfully, they sought help from medical professionals.
"I remember when they told us that the reason we couldn't conceive was because of my fertility issues, it was hard to take, I was in a daze," recalls Louis.
"I felt 'this is all my fault, I'm the one to blame'. I don't think it necessarily made me feel like I was less of a man, but I still felt I was letting my wife down. She was so supportive but inside, I really struggled. Nothing can prepare you at all."
After five years and five failed attempts at IVF treatment, the couple wondered if their dream of holding their own child would ever be realised.
"It was a very lonely time. In many ways you go through it on your own because you're thinking, 'this is my doing, this is all down to me'."
Initially, friends, family and work colleagues enquired as to when they could expect to hear the patter of tiny feet. Eventually, they stopped asking.
"It's so difficult for men because in Irish society, they don't discuss these things in public," says Helen Browne. "Where women can talk about their fertility problems with friends, you can't imagine a man sitting up at the bar chatting about their fertility issues with others. One of our primary functions as human beings is to reproduce. Many men feel that they are failing in their biological duties if they are unable to father a child.
"Instinctively, they see themselves as the protectors; dealing with failure like this is very difficult – some see it as a lack of masculinity and are choked by self-doubt. This is particularly the case with men from rural backgrounds, where opening up about emotional difficulties is far from the common practice."
The NISIG estimates that men and women are equally vulnerable to infertility – 40pc of the sufferers are men and 40pc women. The remaining 20 pc, they estimate, is caused by a combination of male and female problems, while the reasons for a small percentage of infertility cases go unexplained.
"If fertility issues lie evenly with women and men, why are men's battles kept in the dark? We as a society need to talk much more about male infertility," says Helen.
As Louis struggled to come to terms with his situation and each round of IVF treatment failed, he contacted the NISIG for support and found that speaking to other men going through the same difficulties helped him greatly.
"Just to share the problem with another man helped ease the pain. They could relate to what I was experiencing and vice versa. Contacting the support group really was one of the best moves I ever made." Having already spent nearly €50,000 on fertility treatment, Louis and his wife decided to have one last go in early 2013.
They wondered if they were just setting themselves up for more disappointment and heartbreak. Louis' wife was soon to turn 40 and they knew this was their last chance, but the couple's determination drove them forward.
Their persistence paid off.
"When we were told we'd conceived, we froze. There was no feeling of euphoria. We had become so anxious. We had been used to so much disappointment, we just wanted everything to go smoothly."
There was double-joy when the couple were told they were to have twins and in April of this year, the longest of waits finally had the perfect ending.
"To hold them, these perfect little babies in our arms was amazing – beyond words. I still have to pinch myself that this emotional roller coaster finally had a happy ending. I find myself staring at pictures of them on my mobile phone when I'm away from them. I can't get them out of my mind for a second.
"For men out there who feel hopeless, please don't give up. If it came right for us, it can come right for you too. There's always hope."
At the NISIG, men who've gone through similar journeys to Louis can speak directly with those who contact the support group.
"I think men need to speak to other men to truly be helped with this situation," says Helen.
She advises wives and partners to "reassure your other half that you love him so much and that you'll take this journey together.
"Try to get him to relax; reflexology can help. Don't be afraid to use counselling – it can be a great help – and keep talking to him, reminding him that you will both get through this one way or another."
On Sunday, Louis will wake to hear his little babies gurgling and cooing – Father's Day is finally one he can cherish and the agonising days when it seemed like he would never see those twinkling eyes staring back at him, have already become a distant memory.
For those who haven't yet been so fortunate, help and support is available and perhaps this is the perfect weekend to pick up the telephone to speak with someone who knows what you're going through.
*Name has been changed
Lifestyle can affect infertilityLifestyle changes can better men's odds of a successful conception.
1. Decrease drinking Alcohol can reduce the production of normally-formed sperm needed for a successful pregnancy. So if you're trying to conceive, try to cut down.
2. Stop smoking: Low sperm counts and sluggish motility (movement) have been linked to smoking.
3.Watch what you eat Both overweight and underweight men can have fertility problems. With too much weight, there can be hormonal disturbances, and when a man's too lean, he can have decreased sperm count and functionality.
4. Exercise (but in moderation): Excessive exercise could lower your sperm count indirectly by lowering the amount of testosterone in your body.
5. Vitamins help Low levels of vitamin C and zinc can cause sperm to clump together, so keep your numbers up. Vitamin E can counteract excess free-oxygen radicals, which can also affect sperm quality.
6.Limit exposure to toxins Men who have regular contact with environmental toxins or poisons (pesticides, insecticides, lead, radiation, or heavy metals) are at risk of infertility – avoid when and where possible.
7. Try to keep stress levels in check Researchers believe severe stress can affect some men's sperm count. It does this by lowering levels of a hormone called gonadotropin, which is needed for sperm production.
- See more at: http://www.independent.ie/life/health-wellbeing/health-features/what-can-be-done-for-male-infertility-30350454.html#sthash.n9G9iFzI.dpuf
But for Irish men everywhere, the day will serve as a reminder of their difficulties in becoming fathers themselves.
"For many men, not being able to father a child is one of the biggest struggles they will face in their lifetime," says Helen Browne of the National Infertility Support and Information Group (NISIG). "Male infertility is often overlooked in favour of the emotional and physical toll fertility treatment takes on women. Often the men suffer in silence."
When Louis and his wife, who live in the midlands, married seven years ago, they planned to have a family. But, after two years of trying unsuccessfully, they sought help from medical professionals.
"I remember when they told us that the reason we couldn't conceive was because of my fertility issues, it was hard to take, I was in a daze," recalls Louis.
"I felt 'this is all my fault, I'm the one to blame'. I don't think it necessarily made me feel like I was less of a man, but I still felt I was letting my wife down. She was so supportive but inside, I really struggled. Nothing can prepare you at all."
After five years and five failed attempts at IVF treatment, the couple wondered if their dream of holding their own child would ever be realised.
"It was a very lonely time. In many ways you go through it on your own because you're thinking, 'this is my doing, this is all down to me'."
Initially, friends, family and work colleagues enquired as to when they could expect to hear the patter of tiny feet. Eventually, they stopped asking.
"It's so difficult for men because in Irish society, they don't discuss these things in public," says Helen Browne. "Where women can talk about their fertility problems with friends, you can't imagine a man sitting up at the bar chatting about their fertility issues with others. One of our primary functions as human beings is to reproduce. Many men feel that they are failing in their biological duties if they are unable to father a child.
"Instinctively, they see themselves as the protectors; dealing with failure like this is very difficult – some see it as a lack of masculinity and are choked by self-doubt. This is particularly the case with men from rural backgrounds, where opening up about emotional difficulties is far from the common practice."
The NISIG estimates that men and women are equally vulnerable to infertility – 40pc of the sufferers are men and 40pc women. The remaining 20 pc, they estimate, is caused by a combination of male and female problems, while the reasons for a small percentage of infertility cases go unexplained.
"If fertility issues lie evenly with women and men, why are men's battles kept in the dark? We as a society need to talk much more about male infertility," says Helen.
As Louis struggled to come to terms with his situation and each round of IVF treatment failed, he contacted the NISIG for support and found that speaking to other men going through the same difficulties helped him greatly.
"Just to share the problem with another man helped ease the pain. They could relate to what I was experiencing and vice versa. Contacting the support group really was one of the best moves I ever made." Having already spent nearly €50,000 on fertility treatment, Louis and his wife decided to have one last go in early 2013.
They wondered if they were just setting themselves up for more disappointment and heartbreak. Louis' wife was soon to turn 40 and they knew this was their last chance, but the couple's determination drove them forward.
Their persistence paid off.
"When we were told we'd conceived, we froze. There was no feeling of euphoria. We had become so anxious. We had been used to so much disappointment, we just wanted everything to go smoothly."
There was double-joy when the couple were told they were to have twins and in April of this year, the longest of waits finally had the perfect ending.
"To hold them, these perfect little babies in our arms was amazing – beyond words. I still have to pinch myself that this emotional roller coaster finally had a happy ending. I find myself staring at pictures of them on my mobile phone when I'm away from them. I can't get them out of my mind for a second.
"For men out there who feel hopeless, please don't give up. If it came right for us, it can come right for you too. There's always hope."
At the NISIG, men who've gone through similar journeys to Louis can speak directly with those who contact the support group.
"I think men need to speak to other men to truly be helped with this situation," says Helen.
She advises wives and partners to "reassure your other half that you love him so much and that you'll take this journey together.
"Try to get him to relax; reflexology can help. Don't be afraid to use counselling – it can be a great help – and keep talking to him, reminding him that you will both get through this one way or another."
On Sunday, Louis will wake to hear his little babies gurgling and cooing – Father's Day is finally one he can cherish and the agonising days when it seemed like he would never see those twinkling eyes staring back at him, have already become a distant memory.
For those who haven't yet been so fortunate, help and support is available and perhaps this is the perfect weekend to pick up the telephone to speak with someone who knows what you're going through.
*Name has been changed
Lifestyle can affect infertilityLifestyle changes can better men's odds of a successful conception.
1. Decrease drinking Alcohol can reduce the production of normally-formed sperm needed for a successful pregnancy. So if you're trying to conceive, try to cut down.
2. Stop smoking: Low sperm counts and sluggish motility (movement) have been linked to smoking.
3.Watch what you eat Both overweight and underweight men can have fertility problems. With too much weight, there can be hormonal disturbances, and when a man's too lean, he can have decreased sperm count and functionality.
4. Exercise (but in moderation): Excessive exercise could lower your sperm count indirectly by lowering the amount of testosterone in your body.
5. Vitamins help Low levels of vitamin C and zinc can cause sperm to clump together, so keep your numbers up. Vitamin E can counteract excess free-oxygen radicals, which can also affect sperm quality.
6.Limit exposure to toxins Men who have regular contact with environmental toxins or poisons (pesticides, insecticides, lead, radiation, or heavy metals) are at risk of infertility – avoid when and where possible.
7. Try to keep stress levels in check Researchers believe severe stress can affect some men's sperm count. It does this by lowering levels of a hormone called gonadotropin, which is needed for sperm production.
- See more at: http://www.independent.ie/life/health-wellbeing/health-features/what-can-be-done-for-male-infertility-30350454.html#sthash.n9G9iFzI.dpuf
Hidden No More: The Hidden Emotions of Infertility
Infertility affects approximately 10% of the population. Since infertility strikes diverse groups-affecting people from all socioeconomic levels and cutting across all racial, ethnic and religious lines- chances are great that a friend, relative, neighbor or perhaps you are attempting to cope with the medical and emotional aspects of infertility.
Infertility is a major life crisis for 1 in 8 couples. For these women and men fighting the disease of infertility, the infertility experience involves many hidden losses for the individuals, their loved ones and society as a whole, including:
The Hidden Effects of Infertility on Self-Esteem and Relationships
Infertility has a strong impact on self-esteem. Suddenly your life, which may have been well-planned and successful, seems out-of-control. Not only is your physical body not responding as expected but it feels as if your entire life is on hold. Facing the disappointment of not becoming pregnant month after month can lead to depression for both you and your spouse. It’s important to understand the signs of depression. Read more by clicking here.
What can you do?
Pregnancy After Infertility
Congratulations! Transitioning from Your Fertility Specialist to Your Ob/Gyn
I'm Pregnant, Now What?
“Your test results are positive, congratulations, you’re pregnant”. It is everything that you wished for and spent years trying to achieve. You are shocked, elated, scared, tearful, joyful and in disbelief. Now what?
Prior to infertility, your identity was likely defined by your role in your family, your marriage, your work, your interests and hobbies, and your friends. When you found out that you were infertile, your identity and life became increasingly defined by your infertility. If you experienced years of infertility treatments, chances are that your life resolved around your treatment cycles, your moods and your disappointments. As friends of yours became pregnant, you found it increasingly difficult to socialize with them because of your envy. The more years of infertility treatment you experienced, the more isolated you became until you didn’t know who you were apart from your identity as an “infertile.”
Then, seemingly overnight, you find out that you have crossed over to the other side. Pregnancy after infertility brings with it all the normal concerns that a non-assisted pregnancy brings, but adds other layers of emotional complexity. The first challenge is to get over the shock and disbelief of actually being pregnant. During this phase your identity must shift from “infertile” to “fertile.” The emotional and financial resources expended trying to get pregnant can often create a deep seeded fear of losing the pregnancy or of something going wrong with the baby’s development. These fears prevent a couple from sharing their pregnancy news until the second trimester when the greatest possibility of miscarriage has passed. Ironically, like your feelings during your infertility journey, this can be a very lonely, frightening and isolating time for some couples.
If the couple has friends who are also struggling with infertility, then becoming pregnant will pose a challenge to those relationships. It is not uncommon for the pregnant couple to feel guilty that they are successful, but their friends are not. Be prepared, oftentimes these relationships end until all concerned are on their way toward building a family.
One of the most difficult aspects of pregnancy after infertility is rarely spoken about publicly. Pregnancy can be an extremely unpleasant experience for some people, both physically and mentally. After years of ART and yearning for a child, you are expected to be grateful for whatever pregnancy brings and not to complain about it. Hormones are widely implicated in a woman’s sense of well-being. During pregnancy, certain hormones are at an all-time high. For some women, this increase in hormonal level brings with it mental and emotional instability. It is possible to experience high levels of anxiety, depression or both. Understandably, the incongruity of a woman’s fantasies of pregnancy and her experience may cause additional emotional distress.
Pregnancy after infertility is a blessing and a hard won achievement. Your identity shifts from an infertile couple to parents-to-be. Your worries and anxiety about the pregnancy may be heightened because you know what it took to achieve this status. You may be guilty that you are pregnant when your other infertile friends are still struggling. You may be reluctant to even share your pregnancy with others until you feel fairly confident that it is going to last. You may experience physical and emotional symptoms that you did not bargain for when you became pregnant.
It is important that you honor and respect the feelings you have when you become pregnant after struggling with infertility. This is your pregnancy. There is no right or wrong way to feel about it. If you find that your emotions are controlling you however, then working with a professional who is experienced with infertility can be helpful to allay your fears.
Infertility affects approximately 10% of the population. Since infertility strikes diverse groups-affecting people from all socioeconomic levels and cutting across all racial, ethnic and religious lines- chances are great that a friend, relative, neighbor or perhaps you are attempting to cope with the medical and emotional aspects of infertility.
Infertility is a major life crisis for 1 in 8 couples. For these women and men fighting the disease of infertility, the infertility experience involves many hidden losses for the individuals, their loved ones and society as a whole, including:
- Loss of the pregnancy and the birth experience;
- Loss of a genetic legacy and loss of future contributing citizens to the next generation;
- Loss of the parenting experience;
- Loss of a grandparent relationship;
- Low feelings of self-worth;
- Loss of stability in family and personal relationships;
- Loss of work productivity; and
- Loss of a sense of spirituality and sense of hope for the future.
The Hidden Effects of Infertility on Self-Esteem and Relationships
Infertility has a strong impact on self-esteem. Suddenly your life, which may have been well-planned and successful, seems out-of-control. Not only is your physical body not responding as expected but it feels as if your entire life is on hold. Facing the disappointment of not becoming pregnant month after month can lead to depression for both you and your spouse. It’s important to understand the signs of depression. Read more by clicking here.
What can you do?
- Connect with others - find a RESOLVE Support Group
- Learn ways to connect with your partner
- Send information to your family and friends
- Find a mental health expert in your area
Pregnancy After Infertility
Congratulations! Transitioning from Your Fertility Specialist to Your Ob/Gyn
I'm Pregnant, Now What?
“Your test results are positive, congratulations, you’re pregnant”. It is everything that you wished for and spent years trying to achieve. You are shocked, elated, scared, tearful, joyful and in disbelief. Now what?
Prior to infertility, your identity was likely defined by your role in your family, your marriage, your work, your interests and hobbies, and your friends. When you found out that you were infertile, your identity and life became increasingly defined by your infertility. If you experienced years of infertility treatments, chances are that your life resolved around your treatment cycles, your moods and your disappointments. As friends of yours became pregnant, you found it increasingly difficult to socialize with them because of your envy. The more years of infertility treatment you experienced, the more isolated you became until you didn’t know who you were apart from your identity as an “infertile.”
Then, seemingly overnight, you find out that you have crossed over to the other side. Pregnancy after infertility brings with it all the normal concerns that a non-assisted pregnancy brings, but adds other layers of emotional complexity. The first challenge is to get over the shock and disbelief of actually being pregnant. During this phase your identity must shift from “infertile” to “fertile.” The emotional and financial resources expended trying to get pregnant can often create a deep seeded fear of losing the pregnancy or of something going wrong with the baby’s development. These fears prevent a couple from sharing their pregnancy news until the second trimester when the greatest possibility of miscarriage has passed. Ironically, like your feelings during your infertility journey, this can be a very lonely, frightening and isolating time for some couples.
If the couple has friends who are also struggling with infertility, then becoming pregnant will pose a challenge to those relationships. It is not uncommon for the pregnant couple to feel guilty that they are successful, but their friends are not. Be prepared, oftentimes these relationships end until all concerned are on their way toward building a family.
One of the most difficult aspects of pregnancy after infertility is rarely spoken about publicly. Pregnancy can be an extremely unpleasant experience for some people, both physically and mentally. After years of ART and yearning for a child, you are expected to be grateful for whatever pregnancy brings and not to complain about it. Hormones are widely implicated in a woman’s sense of well-being. During pregnancy, certain hormones are at an all-time high. For some women, this increase in hormonal level brings with it mental and emotional instability. It is possible to experience high levels of anxiety, depression or both. Understandably, the incongruity of a woman’s fantasies of pregnancy and her experience may cause additional emotional distress.
Pregnancy after infertility is a blessing and a hard won achievement. Your identity shifts from an infertile couple to parents-to-be. Your worries and anxiety about the pregnancy may be heightened because you know what it took to achieve this status. You may be guilty that you are pregnant when your other infertile friends are still struggling. You may be reluctant to even share your pregnancy with others until you feel fairly confident that it is going to last. You may experience physical and emotional symptoms that you did not bargain for when you became pregnant.
It is important that you honor and respect the feelings you have when you become pregnant after struggling with infertility. This is your pregnancy. There is no right or wrong way to feel about it. If you find that your emotions are controlling you however, then working with a professional who is experienced with infertility can be helpful to allay your fears.

Here’s the truth that very few people know about long distance relationships: No sexuality equals just friends. In this guide, you’ll discover the secrets about sex and seduction that will turn your LDR into a fun, sexy and pleasurable experience.
Discover how to overcome her shyness, how to get her enthusiastic about online sex, how often to bring up sex, and more than 15 creative and fun ideas to spice up your sexual life from distance.
Price: 9$
Discover how to overcome her shyness, how to get her enthusiastic about online sex, how often to bring up sex, and more than 15 creative and fun ideas to spice up your sexual life from distance.
Price: 9$
Wealth Communications Inc. All Rights Reserved






















 RSS Feed
RSS Feed